|
 |
- Search
| J Korean Acad Psychiatr Ment Health Nurs > Volume 31(4); 2022 > Article |
|
Abstract
Purpose
This integrative review aims to identify changes in people with schizophrenia during the COVID-19 pandemic.
Methods
An integrative literature review method of Whittemore and Knafl was applied to integrate the studies. The literature search was conducted in six electronic databases using English and Korean search terms. Three researchers independently reviewed the extracted papers and rated their quality based on predetermined inclusion and exclusion criteria. A total of fifteen relevant studies were included.
Results
The selected articles were all international papers, and most of them were quantitative studies. The changes observed in people with schizophrenia were summarized as follows: (1) changes in health outcomes: psychosocial (increased levels of depression, stress, anxiety, sleep disturbance, and psychotic-like experience) and physical (reduction in food intake, weight loss, changes in immunerelated clinical values, etc.); (2) changes in treatment and health management: increased hospitalization, decreased ICU hospitalization, and a decrease in outpatient visits and prescription rate.
2020년 3월 11일 세계보건기구(World Health Organization)에서 COVID-19 (Coronavirus disease-2019) 팬데믹을 선언한 이후[1], 전세계가 의료뿐만 아니라 사회 · 경제 · 교육 · 문화 등 삶의 전반에서 큰 변화를 경험하였고, 그 영향은 현재까지 지속되고 있다. 특히 질환 등의 장애가 있는 경우에는 이러한 위기 상황에 더욱 심화된 사회경제적 불평등에 놓이게 되어 더 큰 어려움을 겪게 된다[2]. 우리나라에서 COVID-19로 인한 최초의 사망자가 조현병 환자였고, 첫 집단감염의 사례가 만성 정신병원인 청도 대남병원이었던 것이 이러한 재난 불평등을 방증한다[3]. ‘재난약자’란 위험을 감지하는 능력 또는 위험 감지 시 적절한 행동을 하기 어려운 자, 위험을 알리는 정보 습득이 어렵거나 정보를 받아도 적절한 행동이 어려운 자로 정의되며, 최근‘재난약자’와‘재난 취약계층’이란 용어가 함께 쓰이고 있다[4]. 조현병 환자와 같은 중증정신질환자는 감염병 재난 상황에서 적절한 대처를 하기에 많은 어려움이 있는 재난 취약계층에 속하기 때문에 이들의 특수성을 이해하고 이들이 겪는 변화에 대한 기초자료를 확보하는 것이 우선적으로 필요하다.
국민건강보험 자료에 따르면 정신질환자의 COVID-19 관련 감염률 및 사망률이 일반인구에 비해 높았고[5], 국외의 경우에도 감염률, 입원율 및 사망률 모두 일반인구에 비해 높게 나타났다[6, 7]. 특히 조현병 환자는 신체면역력 저하, 밀폐된 구조의 장기시설에서의 거주, 인지기능 및 실행능력 저하로 인한 감염예방 필요성에 대한 이해와 대처 정도의 저하, 낮은 COVID-19에 대한 지식 정도 등의 원인으로 COVID-19에 취약하다[3,5,8,9]. 또한 사회적 거리두기의 영향으로 외래 방문율 감소[10,11], 약물치료 중단의 증가[8] 등 치료 비준수의 문제도 발생할 수 있고, 정신재활시설 서비스 중단[12]으로 정신 사회적 중재 제공이 어려워 전반적인 정신증상 관리 및 재활에도 차질이 생길 것으로 예측된다. 따라서 COVID-19와 같은 감염병 재난 상황에서 조현병 환자에게 나타나는 일상의 변화를 통합적으로 확인하고, 그 내용을 반영한 체계적인 돌봄 정책 및 중재 개발이 절실하다.
그러나 국내에서 조현병 및 중증정신질환자와 COVID-19 관련 경험연구는 찾아보기 어렵고, 감염병 재난 상황에서 정신질환과 관련된 다양한 사회적 문제에 대한 논의가 활발하지 못 하다. 2003년 중증급성호흡기증후군(Severe Acute Respiratory Syndrome), 2009년 신종플루(Novel swine-origin influenza A (H1N1)), 2015년 중동 호흡기 증후군(Middle East Respiratory Syndrome, MERS)에 이어 현 COVID-19 팬데믹까지 신종 감염병으로 인한 재난상황은 반복되고 있으며, 언제든 다시 나타날 수 있다. 따라서 COVID-19 팬데믹 이후 출판된 연구들을 통합적으로 고찰하여 추후 반복될 가능성이 있는 다양한 감염병 재난 상황에 대비하기 위한 기초자료를 마련할 필요가 있다.
체계적 문헌고찰과 메타분석이 무작위 임상 시험과 근거의 우선순위를 지나치게 강조하는 반면, 실험연구와 비실험연구를 동시에 포함하는 가장 광범위한 유형의 통합적 고찰(integrative review) 연구방법은 관심 현상을 완전히 이해하기에 적합한 연구방법이다[13]. COVID-19 팬데믹 상황에 조현병 환자 관련 연구가 어디까지 이루어졌는지에 대한 전반적인 정리와 고찰을 하기 위해서는 통합적 고찰 방법이 적합하다.
그러므로 본 연구에서는 ‘COVID-19 팬데믹 상황에서 조현병 환자에게 나타난 변화는 무엇인가?’라는 연구질문을 토대로 국내 ․ 외 COVID-19와 조현병 관련 연구문헌을 통합적으로 고찰하였다. 이 연구의 결과는 감염병 재난 시 조현병 환자 및 중증정신질환자를 위한 체계적인 방역대책 및 중재 계획에 유용하게 활용될 수 있을 것이다.
이 연구의 목적은 Whittemore and Knafl [13]이 제시한 방법에 따라 통합적 문헌고찰을 수행하여 COVID-19 팬데믹 상황에서 조현병 환자에게 나타나는 다양한 측면의 변화를 파악하고자 하는 것이다.
이 연구는 COVID-19 팬데믹 상황에서 조현병 환자에게 나타난 변화를 파악하기 위한 통합적 문헌고찰 연구이다. 전체적인 연구의 절차는 Whittemore와 Knafl의 통합적 문헌고찰 5단계인 연구문제, 문헌검색, 문헌평가, 문헌분석, 결과제시의 순서를 따랐다[13].
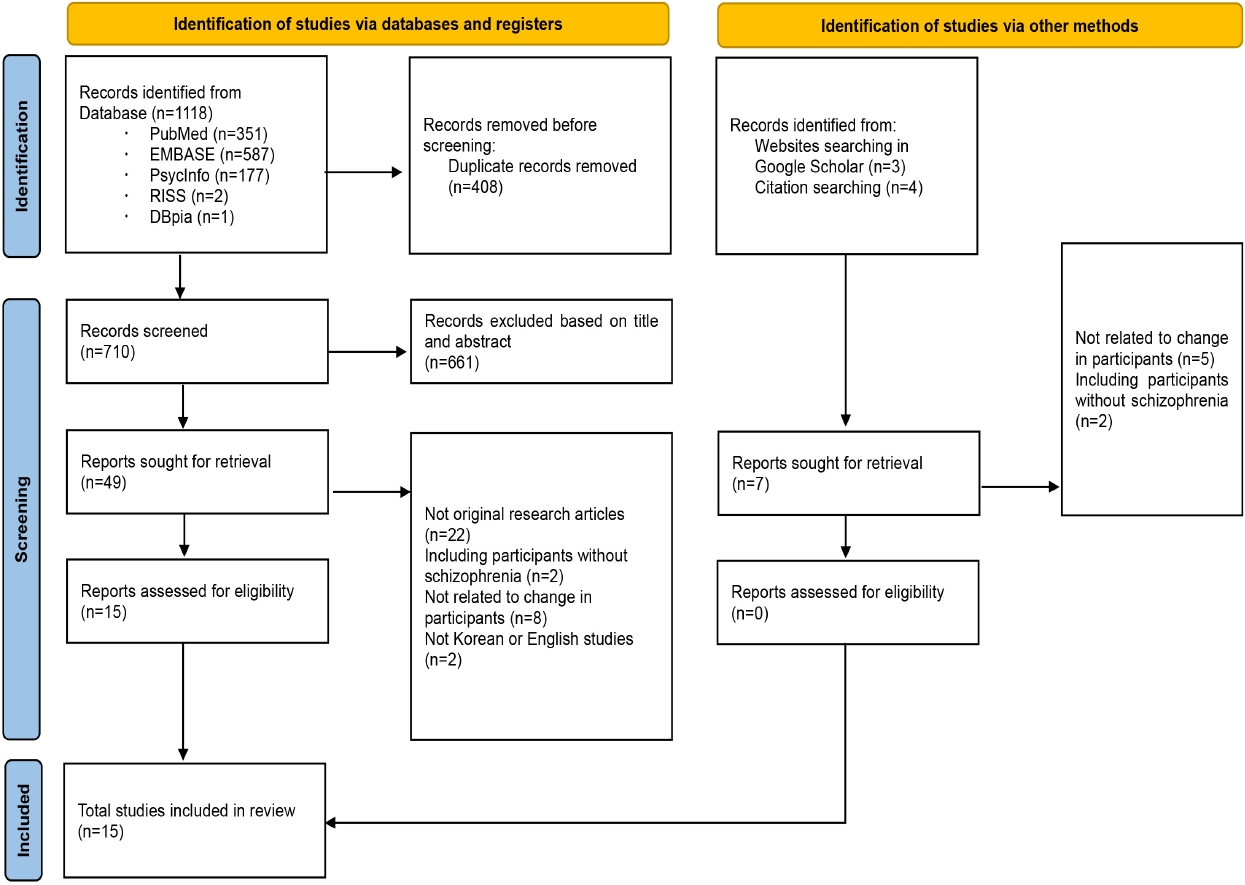
이 연구는 연구자가 속한 기관의 Institutional Review Board로부터 심의면제를 받은 후 시작되었다(IRB NO. DGU IRB 2021028-01). 전반적인 문헌검색과 선정은 3명의 독립된 연구자에 의해 수행되었고, 문헌 선정에서의 이견 등은 연구회의에서 연구자 간 충분한 논의와 의견 수렴을 통해 조정되었다. 문헌검색 전 연구자들이 설정한 문헌 선정기준은 다음과 같다. 1) 2019~2022년 COVID-19 pandemic 기간동안 조현병 환자에게 나타난 변화를 다룬 논문(신종 코로나 바이러스인 ‘2019-nCoV’의 인체감염이 시작된 2019년을 포함), 2) 동료 심사(peer review)를 거친 학술지에 게재된 논문, 3) 한국어 또는 영어로 쓰여진 논문이다. 문헌 고찰에 제외된 논문의 선정 기준은 1) 조현병 환자 이외의 대상자가 포함된 논문, 2) 학위 논문과 편집자 편지, 학술대회 발표, 리뷰 논문 등이었다. 문헌검색은 3명의 독립된 연구자에 의해 2021년 12월 1일부터 2022년 2월 28일에 시행되었다. 국내 검색엔진은 Data Base Periodical Information Academic (DBpia), Research Information Sharing Service (RISS), Korean studies Information Service System (KISS)를, 국외 검색엔진은 EMBASE, PubMed, PsycInfo를 이용하였다. 검색어 선정을 위해 Medical Subject Headings (MeSH)을 활용하였고, 추가로 선행 문헌의 영문제목 및 주요어를 검토하여 다빈도 키워드를 확인하였다. 이에 따라((COVID-19) OR (“COVID 19”) OR (“Coronavirus disease”) OR (“Coronavirus disease-19”) OR (“Coronavirus disease 19”)) AND ((schizophrenia*) OR (“Schizophrenic Disorder”))의 검색식이 수립되었다. 데이터베이스에서 검색된 문헌들은 서지관리 프로그램(EndNote 20.2.1)을 통해 목록화한 후 검토 및 정리하였다. 먼저 각 검색엔진 별 중복문헌을 제거한 후 선정 및 제외기준에 따라 문헌의 제목, 초록, 전문을 단계적으로 검토하였고, 연구자 회의를 통해 최종 분석 대상 문헌을 선정하였다. 국내데이터베이스를 통해 검색된 논문이 부재하여 국외데이터베이스를 통해 검색된 총 1,118편 중 중복문헌이 제거되어 총 710편의 문헌이 추출되었다. 이후 문헌의 선정 및 제외기준에 따라 제목과 초록을 검토한 결과 총 59편의 논문이 추출되었고, 논문 본문을 포함한 전체 내용 검토를 통하여 총 15편의 문헌이 최종 분석 대상으로 선정되었다(Figure 1).
최종 선정된 논문의 질 평가는 Joanna Briggs Institute (JBI) checklists로 실시하였다. Case control study [14], cross sectional study [15], cohort study 연구[16], case report study [17], quasi-experimental study [18], qualitative study [19]에 각각 적용하여 평가하였다. 각 문항은 ‘Yes’, ‘No’, ‘Unclear’ 그리고 ‘Not applicable (NA)’로 응답할 수 있도록 구성되었으며, ‘Yes’로 응답한 경우 JBI의 질 평가 기준을 충족하였음을 의미한다. 15편의 논문을 대상으로 질 평가를 실시한 결과는 Table 1에 제시하였다.
문헌분석 틀은 Microsoft Office사의 Excel 상 매트릭스를 작성하여 분석하였다. 선정된 문헌의 일반적 특성은 연구수행 국가, 연구를 발표한 연도, 연구설계 순으로 분석하였고, COVID-19 팬데믹 기간동안 조현병 환자에게 적용된 접근, 대상자의 특성, 변화 내용 순으로 정리하였다(Table 2). 문헌 분석과 정리는 전체 문헌을 연구자 3인이 독립적으로 검토한 후 통합하는 과정으로 이루어졌고, 분석된 최종 내용에 대해 연구자 간 합의가 도출될 때까지 충분한 논의와 적절성에 대한 재검토를 실시하였다.
문헌고찰을 위해 선정된 15편의 논문을 대상으로 다음과 같은 세 범주의 결과를 도출할 수 있었다.
선정된 문헌들의 일반적 특성은 Table 3과 같다. 분석 대상에 포함된 연구는 총 15편이었고 모두 국외 논문이었다. 연구가 이루어진 단일국가로 중국이 4편(26.67%)으로 가장 많았고, 대륙별로는 유럽연합 국가가 7편(46.67%)으로 나타났다. 출판 연도는 코로나 유행 시기인 2020년부터 2022년까지 분포되어 있었으며 2021년 9편(60.00%)으로 가장 많은 연구가 이루어 졌다. 연구방법은 양적연구(12편)가 우세하였고, 그 중 cross sectional study가 5편(26.66%), case control study와 cohort study 가 각각 3편(20.00%)으로 양적연구의 대부분을 차지하고 있었다.
조현병 환자에게 나타난 건강결과 측면의 변화는 정신사회적 건강 영역과 신체적 건강 영역으로 나뉘어 졌다. COVID-19 팬데믹 상황에서 조현병 환자의 정신사회적 건강 변화를 연구한 다수의 논문에서 대상자의 우울, 스트레스, 불안, 수면 장애의 수준이 증가한 것으로 보고되었다[A1-A4]. 이들 연구는 COVID-19 질병 자체가 주는 불안감과 팬데믹 상황으로 인한 물적, 인적 환경의 변화가 스트레스원으로 작용하여 정신사회적 건강에 영향을 준다고 언급하고 있다.
반면 조현병 관련 양성과 음성 증상의 유의한 변화는 나타나지 않았고[A4], COVID-19의 혼란스러운 상황에서 일반인구와 조현병을 포함한 정신질환자를 비교한 연구에서는 오히려 일반인구에서 정신증상과 유사한 경험이 더 많이 나타났다[A5].
신체적 건강 영역의 변화에서는 조현병 환자들의 음식 섭취 수준 및 체중의 감소 경향이 나타났고[A6], 폐색전증의 발생으로 사망을 한 사례가 보고되었다[A7]. 또한, COVID-19 상황에서 나타난 조현병 환자의 임상검사상의 수치 변화로 염증인자(inflammation markers)(C-reactive protein, fibrinogen 등), 면역 관련 인자(cluster of differentiation 3+ T, cluster of differentiation 4+ T, immunoglobulin M, immunoglobulin G) 등이 정상범위를 벗어난 것으로 확인되었다[A3,A7].
조현병 환자의 COVID-19 치료와 건강관리 측면의 변화를 다룬 연구는 총 8편으로 분석결과를 통합하여 정리하면 다음과 같다. 우선, 조현병 환자의 COVID-19로 인한 입원율은 일반 인구 대비 2배에서 5배 높았으며, 이와 같은 결과는 조현병 환자에 대한 제한적인 초기 의료지원과 의료 불평등의 문제에서 기인된다고 보고되고 있다[A8,A9]. 반면, 중증치료를 위한 중환자실 입원비율은 일반 인구대비 유의한 차이가 없거나 낮은 것으로 나타났다. 이 현상은 대상자를 수용할 병상 가용성, 대상자의 질병 중증도(예. ICU 입원 전 사망), 조현병 환자 스스로의 ICU입원에 대한 선호도 등이 작용한 결과로 해석되고 있다[A10,A11]. 조현병 환자의 사망률의 경우, 높은 비율의 신체 동반질환(예. 비만, 당뇨, 고지혈증, 만성 폐쇄성 폐질환 등), 병원 치료에 대한 접근 지연 등으로 인해 일반 인구대비 3배에서 4배 높은 것으로 나타났다[A9-A11].
한편, 조현병 환자의 감염병 재난 상황에 대한 대처나 치료 참여, 치료기간 측면에서는 일치되지 않는 결과가 확인되었다. 일부 연구에서는 대상자들이 이전과 큰 차이 없이 COVID-19 상황에 잘 대처하며 치료를 받고 있으나[A12], 반면 감염에 대한 불안으로 외래방문을 못하거나 대면상담 없이 또는 온라인 상담 후 처방을 받게 되는 경우가 있었으며[A13], 의사의 처방 횟수 자체가 감소했다는 결과가 보고된 연구도 있었다[A14]. 조현병 환자들의 COVID-19 선별검사의 횟수는 정신과 치료를 위한 사전 검사 등으로 일반 인구대비 많지만 검사 횟수 대비 확진자 수는 적은 것으로 확인되었다[A9]. 또한 COVID-19 양성판정을 받은 집단을 대상으로 진행된 한 연구에서는 조현병 환자의 감염 후 진단까지의 기간과 진단 후 치료까지의 기간이 일반인구에 비해 빨랐다고 보고하기도 하였다[A15].
본 연구는 COVID-19 팬데믹 상황에서 조현병 환자에게 나타난 변화를 확인하여 향후 반복적으로 도래할 수 있는 감염병 재난 상황에서의 조현병 및 정신질환자를 위한 대책과 간호중재를 계획하는 데에 유용한 정보를 제공하기 위해 수행되었다.
본 통합적 고찰에 선정된 최종15편의 연구는 모두 국외 논문이었다. 한국은 COVID-19 팬데믹 초기부터 전 세계로부터 방역 우수국가로 인정받아왔고[20], 보건복지부 산하 국가트라우마센터를 중심으로 재난정신건강 관련 다양한 프로그램을 제공하고 ‘통합심리지원단’을 구성하여 확진자, 자가 격리자, 일반인 등을 위한 적극적인 심리방역을 수행해 온 반면[21], 조현병 및 정신질환자에 대한 특별한 고려 및 관심은 매우 부족하였다. 뿐만 아니라 팬데믹 초기 정신의료기관의 감염병 대책 미비라는 국내 정신의료체계의 한계를 보이며 정신질환자 중 다수의 COVID-19 확진자 및 사망자를 발생시켰다[3]. 정부는 이후 정신건강증진시설의 병상 이격거리 조정, 집단 프로그램 시행의 제한, 손씻기 시설의 의무 설치와 같은 제도의 변화를 추진하였고, 그 결과 팬데믹 초기에 비해 4차 대유행 시기에는 조현병 환자의 COVID-19 확진비율 및 사망자수의 감소추세가 나타났다[22]. 그러나 임상환경을 넘어 지역사회 거주 조현병 대상자에 대한 연구를 바탕으로 이들을 아우르는 감염병 재난에 대한 종합적인 접근은 아직 제시되지 못 하고 있다. 2015년 MERS 유행 시에도 장애인 등의 사회적 약자에 대한 국가적 재난 상황에서의 감염병 관련 지침이나 매뉴얼 마련에 대한 요구가 있었으나 현재까지 부재한 실정이다[23]. 본 통합적 고찰에서 확인된 내용을 포함하여, 추가로 다양한 연구방법론을 활용한 다수의 연구를 통해 조현병 및 정신질환자를 위한 감염병 재난 관련 지식을 축적하고, 다각도의 통합적인 정책을 조속히 마련하여 감염병 재난에 대비할 필요가 있다.
한편 분석된 15편 중 12편이 양적연구방법으로 수행되었는데, COVID-19 팬데믹 상황에서 조현병 환자의 가족 돌봄 경험을 연구한 선행연구에 따르면 조현병 환자의 증상 단계별로 건강관리 및 재활, 그리고 요구 사항이 상이하였다[24]. 따라서 조현병 환자가 참여하는 추가의 질적연구를 통해 팬데믹에서의 개별적인 경험을 깊이 있게 탐색하여 마스크 착용, 사회적 거리두기 등 비장애인 중심의 방역환경에서 이들이 조현병을 지닌 채 어떻게 지내왔는지를 확인하는 것은 더욱 실효성 있는 중재 개발에 도움이 될 것으로 사료된다.
또한 본 연구의 문헌 검색 기간은 2022년 2월 28일까지였고, 우리나라에 중증도와 사망률이 상대적으로 낮은 오미크론 변이가 출연하여 5차 유행이 시작되던 시점이었다[25]. 이후 신규확진자의 수는 더욱 증가하였으나 백신 접종률이 증가하고 단계적 일상회복을 시작하는 엔데믹 단계에 접어들었다. 따라서 이러한 국면 전환이 조현병 환자에게 어떠한 변화를 일으켰는지 이후의 연구들을 분리하여 통합해 볼 필요가 있겠다.
COVID-19 팬데믹 상황에서 조현병 환자들에게 나타난 정신사회적 건강의 변화는 우울, 스트레스, 불안, 수면 장애의 수준이 증가한 것으로 무력감, 우울감이 심화되었다는 선행연구와 일치하는 결과이다[24]. 그러나 앞선 선행연구[24]에서는 정신증상도 악화되어 재입원이 증가하였다고 보고한 반면, 본 연구에서 분석된 연구 중에는 양성 또는 음성 증상의 악화가 유의미 하지 않은 것으로 나타났다[A4]. 따라서 COVID-19 팬데믹 상황에서 조현병 환자의 정신증상이 악화된다고 단정지을 수는 없으나 사회적 거리두기 및 여러 공적 조치들로 지역 정신건강증진시설의 역할이 중단 및 축소되면서 타인과의 상호작용 감소에 따라 증가되는 사회적 고립감, 무력감, 우울감 등이 매개하여 정신증상 악화를 야기할 가능성을 고려해 볼 수 있다. Shin과 Joung [24]의 연구에서 조현병 환자를 돌보는 가족들은 팬데믹 상황에서 사회적 거리두기가 중요함에도 불구하고, 소수 인원의 교대 방식과 같은 탄력적 운영, 국가 지원의 근로 지원인의 도움 등을 활용하여 대면 활동을 유지해야 함을 강력하게 주장한 바 있다. 또한 일본의 경우 정신장애인 사업장에서 팬데믹으로 휴관이 장기화되었으나 정신질환이 있는 사람들을 격리시키지 않기 위해 인터넷 미팅 등 비대면 프로그램을 지속하여 관계나 일상의 리듬을 유지하게 하였다[26]. 즉 거리두기가 필요한 감염병 재난 상황에 조현병 환자가 고립되지 않고 돌봄을 지속적으로 제공받을 수 있도록 하기 위해서는 효율적인 대면 ․ 비대면 방법에 대한 개발 및 훈련이 엔데믹 상태로 일상을 회복한 지금부터 바로 추진되어야 하겠다.
한편 신체적 건강 측면에서의 변화는 소수의 대상자 또는 사례를 제시한 연구가 대부분으로 일반화하기에는 어려움이 있는 결과들이었으나 조현병 환자들이 일반 인구에 비해 신체적 면역력 저하[3] 및 신체 질환, 특히 만성질환 이환률이 매우 높은 편이며[27], COVID-19 관련 감염률 및 사망률이 일반인구에 비해 높은 것이[5] 본 연구결과와 일맥상통하다. 또한 본 연구의 분석에 포함된 연구 중에도 COVID-19로 인한 조현병 대상자의 일반 인구 대비 입원율 및 사망률은 높은 것으로 나타났다. 그러므로 감염병 재난 시 조현병 환자의 경우 일반인구에 비해 더 적극적인 방역수칙 준수를 통한 예방이 필요하고, 따라서 체계적인 대처 및 건강관리 교육 프로그램의 개발 및 제공이 선행되어야 하겠다.
또 하나의 주목할 만한 결과는 조현병 환자의 COVID-19 선별검사 비율이 일반인구 대비 높았던 반면, 검사 횟수 대비 확진자 수는 적은 것이다. 이는 정신건강증진시설이나 의료기관 이용 시 검사가 선행되어야 한다는 점에서 그 원인을 찾을 수 있고, 사회적 고립, 독거 등으로 조현병 환자의 전염의 기회는 감소되었을 것으로 추측할 수 있다. 이러한 결과는 조현병 환자의 경우 부정적인 사회 인식으로 인해 COVID-19 팬데믹 이전의 삶이 이후와 다름없는 ‘격리상태’로 위축된 채 살아왔다는 선행연구와 유사한 결과이다[24]. 팬데믹 상황에서 강도높은 사회적 거리두기가 지속될 때 많은 사람들이 변화된 일상에 불안과 우울감을 경험하였다. 이러한 재난 상황을 통해 우리 사회가 더 건강한 방향으로 도약하기 위해 조현병 환자의 삶을 이해하고 관심을 갖게 되는 계기가 될 수 있을 것으로 사료된다. 그러기 위해서는 단순히 취약계층을 위한 사회안전망 확충을 넘어 동일한 시민으로 함께 살아가게 하기 위한 사회 전반의 인식 개선 또한 요구된다[28].
COVID-19 팬데믹 상황에서 조현병 환자의 치료 유지 정도는 연구마다 차이가 있어 합의된 결론을 내리기 어려웠다. 조현병 환자에게 치료 유지는 재발 예방에 강력한 예측요인으로 매우 중요한 이슈이며, 사회적 거리두리 상황이나 감염에 대한 두려움으로 외래 방문에 차질을 빚을 가능성은 존재하나 봉쇄령이 내려졌거나 의료기관과의 접근성이 상대적으로 어려운 국외와 국내는 상황이 다를 것으로 추측되는 바, 추후 국내의 외래 방문율 및 처방율에 대한 정확한 확인이 필요하겠다.
이상으로 본 연구를 통해 COVID-19 팬데믹 상황에서 조현병 환자에게 나타난 변화를 건강결과와 치료 및 건강관리 측면에서 확인하였다. 본 연구의 결과는 팬데믹 상황에서 조현병 환자들에 대한 연구 전반을 통합하여 감염병 재난 상황에서의 조현병 환자들을 위한 대책 마련 및 중재 개발을 위한 근거자료를 마련하였다는 점에서 의의가 있다. 그러나 이 연구는 2022년 2월까지 출판된 연구들을 고찰하였다는 제한점이 있다.
이와 같은 본 연구결과의 의의와 제한점을 기반으로 다음과 같이 제언하고자 한다. 첫째, 2022년 3월 이후 출판된 COVID-19와 조현병 환자 관련 연구에 대한 추가 고찰로 대상자의 변화양상에 대한 추가 확인과 통합이 필요하다. 둘째, 사회적 거리두기 상황에서 조현병 환자들의 고립을 막기 위한 다양하며 실효성 있는 비대면 프로그램의 개발이 필요하다. 셋째, 감염병 재난 상황에 조현병 환자들의 감염 예방을 위한 교육 프로그램이 개발 및 제공되어야 한다. 넷째, 조현병 환자들이 경험한 팬데믹을 깊이 있게 탐색하는 질적연구가 수행되어야 할 것이다.
본 연구는 COVID-19 팬데믹 상황에서 조현병 환자와 관련된 연구를 통합적 고찰 방법으로 탐색하여 감염병 재난 상황에서 그들에게 나타난 변화를 확인하였고, 그 결과는 정신사회적 건강, 신체적 건강 그리고 치료 및 건강관리 측면으로 나타났다. 추후 반복될 가능성이 있는 감염병 재난 상황에 대비하기 위하여 조현병 환자 및 정신질환자를 위한 감염병 관련 지침이나 매뉴얼 마련 등 종합적인 대책 마련이 시급하다. 더불어 팬데믹을 경험한 조현병 환자 대상의 질적연구를 포함한 국내 실정을 반영한 추가의 연구를 통해 증상 단계별로 건강관리, 재활, 요구에 대해 통합적인 탐색이 이루어진다면 더욱 실효성 있는 계획 마련에 도움이 될 것이다. 또한 거리두기가 요구되는 상황에서도 조현병 환자 및 정신질환자들이 치료 및 재활을 지속할 수 있는 비대면 시스템 및 활용 교육이 엔데믹 상황으로 전환된 지금부터 체계적으로 준비되어야 하겠다.
본 연구결과는 간호연구 측면에서 감염병 재난 상황에서의 조현병 환자에 대한 지식이 축적되었다는 점에서 의의가 있고, 간호교육 측면에서는 조현병 환자를 위한 감염병 예방 프로그램을 구성하는 내용을 제시하였고, 마지막으로 간호실무 측면에서 팬데믹 상황에서 나타난 조현병 환자들의 변화를 확인하여 간호중재 제공 시 기초자료가 될 것으로 본다. 본 연구결과를 기반으로 추후 반복될 가능성이 있는 감염병 재난 상황에서의 종합적인 시스템 및 대책 마련이 필요하다.
Notes
AUTHOR CONTRIBUTIONS
Conceptualization or/and Methodology: Joung J
Data curation or/and Analysis: Kang KI, Choi DJ, & Joung J
Funding acquisition: Joung J
Investigation: Kang KI, Choi DJ, & Joung J
Project administration or/and Supervision: Joung J
Resources or/and Software: Kang KI
Validation: Kang KI & Joung J
Visualization: Kang KI
Writing: original draft or/and review & editing: Kang KI, Choi DJ, & Joung J
Table 1.
JBI Critical Appraisal of Included Studies by Research Design
Table 2.
Summary of Studies of Changes Experienced by Patients with Schizophrenia
Table 3.
General Characteristics of the Reviewed of Papers (N=15)
REFERENCES
1. World Health Organization (WHO). WHO Director-General's opening remarks at the media briefing on COVID-19 [Internet]. Geneva: WHO; 2020 [cited 2020 May 6]. Available from: https://www.who.int/dg/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020
2. United Nations, A Disability-Inclusive Response to COVID-19, Police Brief. Newyork: United Nations; 2020. May
3. Kim SW. Supporting patients with schizophrenia in the era of COVID-19. Korean Journal of Schizophrenia Research. 2021;24(2):45-51. https://doi.org/10.16946/kjsr.2021.24.2.45

4. Yim DK. An analysis of helping vulnerable people to disastersfocusing the welfare evacuation-. Asia-pacific Journal of Multimedia Services Convergent with Art, Humanities, and Sociology. 2019;9(5):587-602. https://doi.org/10.35873/ajmahs.2019.9.5.054

5. Seon JY, Kim S, Hong M, Lim MK, Oh IH. Risk of COVID-19 diagnosis and death in patients with mental illness: a cohort study. Epidemiology and Psychiatric Sciences. 2021;30: https://doi.org/10.1017/S2045796021000597

6. Wang Q, Xu R, Volkow ND. Increased risk of COVID-19 infection and mortality in people with mental disorders: analysis from electronic health records in the United States. World Psychiatry. 2021;20(1):124-130. https://doi.org/10.1002/wps.20806


7. Toubasi AA, AbuAnzeh RB, Tawileh HBA, Aldebei RH, Alryalat SAS. A meta-analysis: The mortality and severity of COVID -19 among patients with mental disorders. Psychiatry Research. 2021: 113856 https://doi.org/10.1016/j.psychres.2021.113856

8. Muruganandam P, Neelamegam S, Menon V, Alexander J, Chaturvedi SK. COVID-19 and severe mental illness: impact on patients and its relation with their awareness about COVID-19. Psychiatry research. 2020;291: 113265 https://doi.org/10.1016/j.psychres.2020.113265



9. Pinkham AE, Ackerman RA, Depp CA, Harvey PD, Moore RC. COVID-19-related psychological distress and engagement in preventative behaviors among individuals with severe mental illnesses. NPJ Schizophrenia. 2021;7(1):1-7. https://doi.org/10.1038/s41537-021-00136-5



10. Ryu S, Nam HJ, Baek S-H, Jhon M, Kim JM, Kim SW. Decline in hospital visits by patients with schizophrenia early in the COVID-19 outbreak in Korea. Clinical Psychophamacology and Neuroscience. 2022;20(1):185-189. https://doi.org/10.9758/cpn.2022.20.1.185

11. Seo JH, Kim SJ, Lee M, Kang JI. Impact of the COVID-19 pandemic on mental health service use among psychiatric outpatients in a tertiary hospital. Journal of Affective Disorders. 2021;290: 279-283. https://doi.org/10.1016/j.jad.2021.04.070



12. Melamed OC, Hahn MK, Agarwal SM, Taylor VH, Mulsant BH, Selby P. Physical health among people with serious mental illness in the face of COVID-19: Concerns and mitigation strategies. General Hospital Psychiatry. 2020;66: 30-33. https://doi.org/10.1016/j.genhosppsych.2020.06.013



13. Whittemore R, Knafl K. The integrative review: updated methodology. Journal of Advanced Nursing. 2005;52(5):546-553. https://doi.org/10.1111/j.1365-2648.2005.03621.x


14. JBI. Critical appraisal tools Joanna Briggs Institute2020a. Available from: https://jbi.global/sites/default/files/2021-10/Checklist_for_Case_Control_Studies.docx
15. JBI. Critical appraisal tools 2020b. Available from: https://jbi.global/sites/default/files/2021-10/Checklist_for_Analytical_Cross_Sectional_Studies.docx
16. JBI. Critical appraisal tools 2020c. Available from: https://jbi.global/sites/default/files/2021-10/Checklist_for_Cohort_Studies.docx
17. JBI. Critical appraisal tools Joanna Briggs Institute 2020a. Available from: https://jbi.global/sites/default/files/2021-10/Checklist_for_RCTs.docx
18. JBI. Critical appraisal tools 2020b. Available from: https://jbi.global/sites/default/files/2021-10/Checklist_for_Case_Reports.docx
19. JBI. Critical appraisal tools 2020c. Available from: https://jbi.global/sites/default/files/2021-10/Checklist_for_Qualitative_Research.docx
20. UN News. First person: South Korea's COVID-19 success story. [Internet]. 2020 [cited 2020 May 1]. Available from: https://news.un.org/en/story/2020/05/1063112
21. Choi J. The Effects of COVID-19 Pandemic on the Mental Health of the General Public and Children and Adolescents and Supporting Measures. Journal of the Korean Neuropsychiatric Association. 2021;60(1):2-10. https://doi.org/10.4306/jknpa.2021.60.1.2

22. National Center for Mental Health. Group infections in mental health promotion facilities and response status. Paper presented at: Symposium on Improving Mental Health Services in the context of the COVID-19 Pandemic; 2021. December 14; Seogang University. Seoul
23. Kang H. MERS lawsuit 3 years…The Ministry of Health and Welfare rejects the court's mediation plan to "prepare safety measures against infectious diseases for the disabled". Beminor. 2019 March 26;Sect.01
24. Shin S, Joung J. Family members' caring experiences of Schizophrenia patients during the COVID-19 pandemic: deepened disconnection due to distancing. Journal of Korean Academy of Psychiatric and Mental Health Nursing. 2022;31(3):293-303. https://doi.org/10.12934/jkpmhn.2022.31.3.293

25. Kim YW, Kim YM, Lee SM, Im JH, Im DS, Park YJ. Analysis of COVID-19 confirmed cases and their cohabitants and related factors during the period of Omicron dominance. Weekly Health and Illness; 2022. Available from: https://www.kdca.go.kr/board/board.es?mid=a20602010000&bid=0034&list_no=719295&act=view
26. Shin J. Multilayered disasters and pandemic solidarity: based on the interviews with disability activists and nurses in the pandemic of Korea and Japan. Critical Review of History. 2020;132: 121-164.

27. Leucht S, Burkard T, Henderson J, Maj M, Sartorius N. Physical illness and schizophrenia: a review of the literature. Acta Psychiatrica Scandinavica. 2007;116: 317-333. https://doi.org/10.1111/j.1600-0447.2007.01095.x


28. Jeon GB. Qualitative case study on the self-quarantine experience of disabled activist during the COVID-19 crisis. Journal of Korean Disability Studies. 2020;5(2): 51-85.